Checklist for Evaluating Dementia Care Facility Safety
A practical checklist for evaluating memory care safety: physical environment, wandering prevention, emergency plans, staff training, meds, activities, and red flags.

When choosing a dementia care facility, safety should be your top priority. Individuals with dementia face unique risks, such as wandering, falls, and difficulty communicating concerns. This guide helps you evaluate facilities effectively, covering key areas like:
- Physical Safety: Check for non-slip flooring, good lighting, handrails, and secure outdoor spaces.
- Wandering Management: Look for secured doors, anti-wandering technology, and restricted access to hazardous areas.
- Emergency Preparedness: Ensure fire safety measures, evacuation plans, and response systems are in place.
- Staff Training: Verify if caregivers are trained in dementia-specific care and medication management.
- Resident Engagement: Review activity schedules, personalized living spaces, and communal areas.
- Red Flags: Watch for signs of neglect, high staff turnover, or poor maintenance.
With memory care costs averaging $6,450/month, it's crucial to visit facilities, ask questions, and review inspection reports. This checklist ensures your loved one’s safety and quality of care.
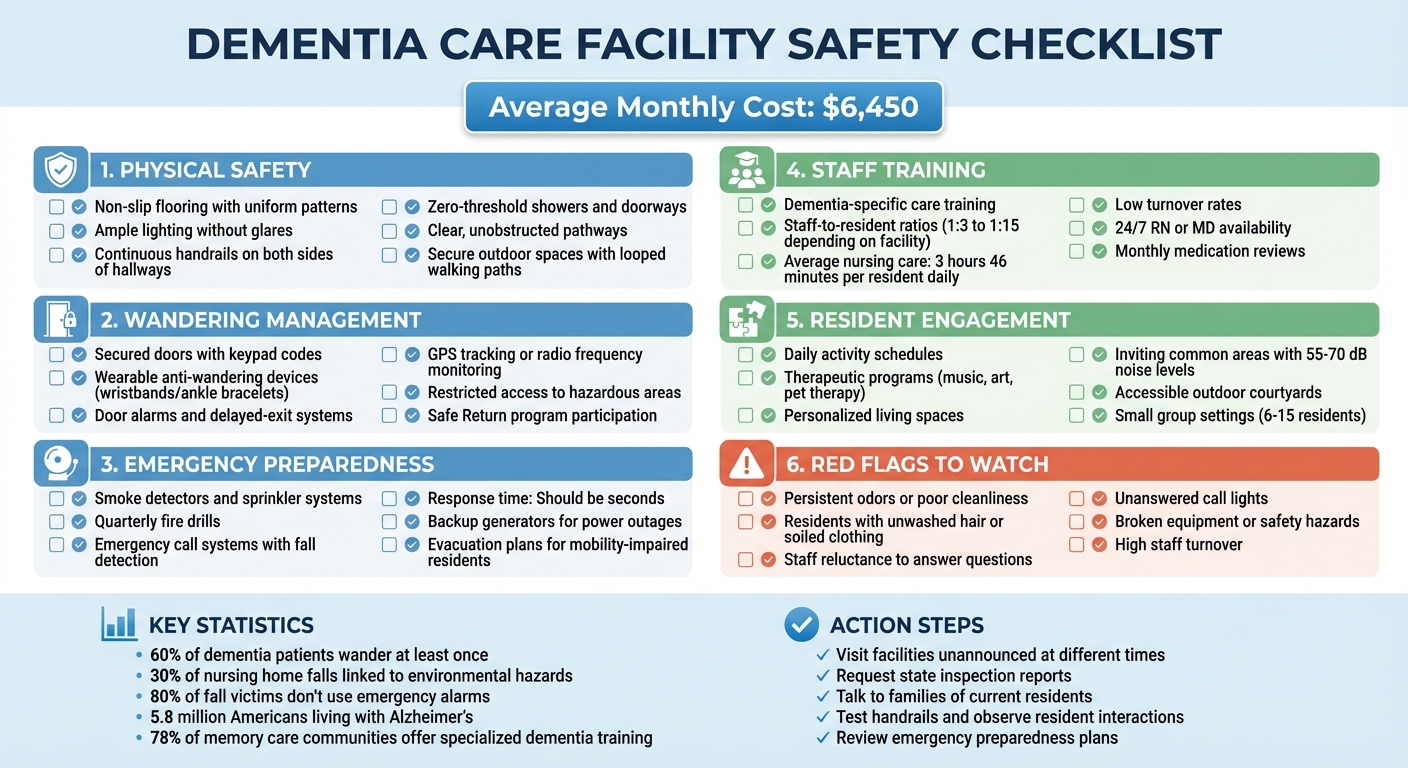
Dementia Care Facility Safety Evaluation Checklist
Assisted Living Safety Dementia Patient and ADLS
Physical Environment and Accessibility
Creating a safe and accessible physical environment is a crucial step in ensuring the well-being of residents in dementia care facilities. With over 30% of nursing home falls linked to environmental hazards, careful attention to design can significantly improve safety.
Fall Prevention Design Features
Start with flooring. Non-slip surfaces with simple and uniform patterns are ideal. Avoid high-contrast or intricate designs on carpets and tiles, as these can confuse residents with dementia, who might perceive them as obstacles or gaps, leading to hesitation or even falls. Opt for plain or subtly mottled patterns to minimize visual misinterpretations.
Lighting is another key factor. Ample natural light helps residents stay oriented, but it’s important to avoid harsh glares or deep shadows. Motion-activated night lights can further enhance safety, especially for nighttime trips to the bathroom.
Keep pathways clear and unobstructed. Install continuous handrails on both sides of hallways to assist with navigation. Professor Andrew Clark from the University of Greenwich highlights the importance of thoughtful design:
"Environment is really important, and it can be enabling or disabling. We need to find ways for people to connect, to maintain routines and everyday activities".
Check for uneven flooring, broken tiles, or abrupt transitions between surfaces. These can be tripping hazards for residents. Features like zero-threshold showers and doorways - where there are no raised edges - are particularly effective in reducing falls. Observe how residents move through the space. Do they hesitate at floor transitions or struggle in dim lighting? These behaviors can reveal problem areas.
Emergency Exits and Accessibility Features
Emergency exits should combine security with ease of use. Clear markings with simple visual cues are essential to guide residents during evacuations. Vicky Gemme, writing for ECDOL, underscores this point:
"Safety-conscious design is one of the most important aspects of memory care. Look for features that support orientation, reduce confusion, and prevent wandering".
Ensure that handrails are sturdy and that pathways are wide enough to accommodate mobility devices, especially during emergencies when multiple residents may need to evacuate at once. TerraBella Senior Living also emphasizes:
"The physical layout of the memory care home should cater to the specific needs of residents. Safe living spaces, including wide hallways, non-slip flooring, and well-lit rooms, help reduce the risk of falls and injuries".
Ask to see the facility's most recent state inspection report for any noted deficiencies in fire safety or exit accessibility. Additionally, inquire about evacuation plans for residents with limited mobility and confirm the presence of alert systems or call buttons throughout the building to ensure residents can signal for help when needed.
Outdoor Space Safety
Secure outdoor areas provide therapeutic value while maintaining safety. Research shows that access to outdoor spaces can reduce agitation and aggression in people with dementia. It also promotes safe sun exposure, which is beneficial for vitamin D levels and bone health.
Fencing should be discreet yet secure, with non-climbable designs. Gates should feature hidden handles and latches to prevent wandering. All plants in the area should be non-toxic, and trees should not be close enough to allow climbing.
Continuous walking paths that loop back to the starting point are especially helpful, as they allow residents to walk independently without encountering dead ends. These paths should include handrails and, where possible, raised garden beds that are accessible to those in wheelchairs or seated positions.
Outdoor furniture should be stable, have rounded edges, and resist extreme temperatures to ensure comfort and safety. Shaded seating areas, such as those with gazebos or umbrellas, provide relief from the sun while reducing glare. Motion-activated lights can keep outdoor pathways well-lit after dark. Lastly, secure all gardening tools, chemicals, and fertilizers in locked storage to prevent accidents.
These thoughtful design features not only enhance safety but also contribute to a supportive environment where residents can thrive, both indoors and outdoors.
Wandering Management and Security Systems
When it comes to dementia care, ensuring resident safety is paramount. One key aspect of this is managing wandering - a behavior that affects about 60% of individuals with dementia at least once. This makes having effective security measures an absolute must for any reputable dementia care facility.
Secured Entrances and Exits
Facilities need to ensure that every exterior door is equipped with safeguards like keypad codes or staff-assisted access. Locks should be installed out of residents' easy reach to minimize the risk of unsupervised exits. As the California Advocates for Nursing Home Reform points out:
"Dementia care is often characterized by locked doors or otherwise secured perimeters to prevent residents from leaving the facility unsupervised".
During a facility visit, ask for a demonstration of door alarms to see how quickly they respond with both audible and electronic alerts. Look for delayed-exit systems that momentarily secure doors during an attempted exit. Outdoor spaces should also be enclosed with secure fencing and gates, allowing residents to enjoy fresh air without compromising safety.
In addition to physical barriers, advanced technology plays a vital role in preventing wandering incidents.
Anti-Wandering Technology
Modern dementia care facilities often use multiple layers of monitoring technology. Wearable devices - such as wristbands, ankle bracelets, or ID bracelets - are common tools that trigger alarms when residents approach restricted perimeters. Highgate Senior Living explains:
"Some places might have alarms on the elevators and doors, while other dementia care facilities might have residents wear wrist or ankle bracelets that set off alarms if they leave the unit".
Ask about the specific technologies in use. For instance, GPS tracking provides real-time location updates, while radio frequency systems monitor movement within the facility's boundaries. It's also important to confirm how often wearable devices are maintained to ensure they function properly at all times.
Additional measures like pressure-sensitive mats, motion sensors, or even door camouflage can further reduce wandering risks. When touring a facility, request to see these systems in action to understand how they work.
Restricted Access to Hazardous Areas
Certain areas - such as kitchens, laundry rooms, medication storage, and maintenance spaces - should be off-limits to residents unless supervised. These spaces should either remain locked or use keypad controls that residents cannot easily operate. The Sanctuary highlights the importance of such precautions:
"Safety is a top priority, especially for individuals with dementia who may wander or require additional supervision. In large facilities, safety is a concern because there aren't enough eyes on the residents".
Observe whether staff actively supervise residents near service doors or other potentially hazardous areas. Additionally, check if the facility participates in a "Safe Return" program. These programs, which involve registering residents with local law enforcement, can be a critical part of recovering individuals who may wander off the premises. This level of preparedness reflects a strong commitment to safety and peace of mind for families.
Emergency Preparedness and Response
For facilities accepting Medicare and Medicaid, having a solid emergency preparedness plan isn't just a recommendation - it's a requirement. But when it comes to dementia care, a one-size-fits-all plan simply won't work. Residents with cognitive impairments often face challenges like understanding instructions, recognizing dangers, or responding quickly to alarms. This means the plan must be customized to meet their specific needs. By addressing these unique challenges, emergency measures work hand-in-hand with other safety features to ensure quick and effective crisis management.
Fire Safety Measures
Fire safety in a memory care facility goes beyond just having the basics. Essential devices like smoke detectors, alarms, carbon monoxide alarms, and sprinkler systems should be installed and maintained regularly. Emergency exits need to be clearly marked, and fire extinguishers must be both accessible and in good working order. When visiting a facility, don’t hesitate to ask for their written fire safety plan and inquire about the frequency of system inspections.
"Emergency and nurse call systems should be plentiful and working in all public and private areas." - Lakeside Manor
In memory care settings, fire drills are typically conducted quarterly. It’s also a good idea to check state health department inspection reports for any past safety issues, such as malfunctioning sprinkler systems, poorly executed fire drills, or staffing shortages during emergencies.
Emergency Call Systems
Advanced emergency call systems are a must-have in memory care facilities. These include call buttons and wearable alert devices equipped with automatic fall detection, which can notify staff even if the resident doesn’t press a button. This is vital, as studies show that in 80% of reported falls, residents did not use their alarm to request help. Modern facilities now rely on this technology to ensure immediate action.
When evaluating a facility, ask about their average response time to emergency alerts. According to AARP caregiving expert Amy Goyer, a response "should be seconds". Also, confirm that the call systems have two-way communication and backup power to guarantee reliability during outages.
Evacuation and Disaster Planning
Evacuation plans in memory care facilities must account for residents with mobility or memory challenges. Look for details like how they assist residents during evacuations and whether they maintain emergency supplies. Backup generators are also essential to keep medical equipment, electronic records, and climate control functioning during power outages.
Atria Park provides a great example, as they successfully evacuated residents during wildfires in January 2025, showcasing their preparedness.
Barry Zeltzer, CEO of Hattie Ide Chaffee Home, stresses the importance of tailoring plans to meet the needs of residents:
"You must look at your special needs population and determine if they fit into your emergency preparedness plan. If they don't, you'll need to revise that plan for residents with disabilities and cognitive impairment who may require additional assistance."
Ask to review the facility's full emergency preparedness plan - it’s public information and should be easily accessible at nurse stations. Also, inquire about the frequency of staff drills for scenarios like fires, medical emergencies, natural disasters, or security threats. Finally, check if the facility has partnerships with local organizations to assist with evacuations when necessary.
Staff Training and Competency
The quality of dementia care in any facility depends heavily on the training and skills of its staff. Even the best-designed buildings or cutting-edge technology are of little use if caregivers aren't equipped to meet the complex needs of residents with cognitive challenges. Federal guidelines mandate that nurse aides in skilled nursing facilities complete at least 12 hours of annual in-service training, including dementia management. Despite this, only 29% of the social care workforce in England had received dementia training by late 2024.
Dementia-Specific Care Training
When assessing a facility, it’s crucial to ask about the type of dementia training provided to staff and how often it’s updated. Essential training topics include dementia awareness, person-centered care, communication strategies, behavioral management, safeguarding, and end-of-life care [35,36]. Facilities that adopt a tiered training model often stand out. This approach ensures all staff receive basic dementia awareness, while those in regular contact with residents gain enhanced knowledge, and leadership or specialist roles receive advanced training.
Communication skills are a cornerstone of effective dementia care. Training should cover verbal techniques like simplifying instructions into one-step commands and avoiding "elderspeak", alongside non-verbal methods such as appropriate body language and facial expressions. The most impactful training programs blend online resources with interactive elements like face-to-face sessions, role-playing, and video scenarios. These methods help build both empathy and practical skills. Facilities that prioritize live, interactive training over self-paced e-learning often see better outcomes [35,37].
"High-quality mandatory dementia training for the social care workforce is imperative... it highlights the significant benefits that dementia training can bring to people's lives, as well as to the wider health and care system." - Alzheimer's Society
Staffing Ratios and Turnover Rates
Staff-to-resident ratios can vary widely depending on the facility. Larger, institutional settings might have ratios of 1:12 or even 1:15, while smaller, boutique-style facilities may strive for a 1:3 ratio (e.g., two caregivers for every six residents). On average, nursing home residents receive 3 hours and 46 minutes of nursing care per day in the U.S.. When touring a facility, ask for shift-specific ratios, including nights and weekends, to gauge how much individual attention residents receive [40,1,3].
Frequent staff turnover can disrupt the continuity of care, which is especially critical for dementia residents. During your visit, observe whether staff seem calm and engaged or rushed and stressed [29,14]. It’s also worth asking if the facility depends on temporary staffing agencies or employs permanent, full-time staff. Public records, like those on Medicare.gov, can provide insights into staffing levels and turnover rates. Additionally, high turnover among administrators can signal deeper management issues.
"If a facility has churned through several administrators in a few years, that's a troubling sign about the quality of its management and owners." - Jordan Rau, The New York Times
Medication Management Protocols
Proper medication management is critical in dementia care and requires strict protocols and oversight. Psychoactive drugs should only be used as a last resort, as they are often unsuitable for dementia patients. Ask how the facility manages challenging behaviors and whether sedative medications are commonly prescribed. Residents should have their medications reviewed by a physician at least every 30 days to ensure they remain effective.
While touring, pay attention to residents' appearances. Signs like lethargy, listlessness, or stupor could indicate over-medication or misuse of chemical restraints. High-quality facilities ensure a Registered Nurse is always on-site or have a medical doctor available 24/7 for emergencies and medication adjustments [15,40]. Additionally, someone with specialized dementia training should oversee resident assessments and care plans, including medication management.
"Psychoactive drugs are often contraindicated for elderly people with dementia and should only be used as a last resort, if ever." - California Advocates for Nursing Home Reform (CANHR)
Resident Engagement and Quality of Life
Creating a safe environment is crucial, but meaningful engagement is just as important for preserving dignity and enhancing quality of life. With nearly 5.8 million Americans living with Alzheimer's disease, the need for facilities that balance safety with enriching activities has never been greater.
Activities and Stimulation Programs
Take a close look at the facility’s daily activity schedule to ensure there are programs every day. Top-tier facilities often include therapeutic activities like music, art, and pet therapy, alongside cognitive exercises such as puzzles, memory games, and simulated daily tasks. Physical activities like chair-based exercises, dancing, or supervised walks on secure outdoor paths can also play a big role in improving residents' well-being.
"Quality of life should be a number one priority when looking for a memory care facility. A flexible daily schedule full of stimulating programs, exercise, music, and therapies can help your loved ones stay engaged and enjoy their lives."
– Maplewood Senior Living
Ask whether activities are tailored to residents' cognitive levels. For example, are residents grouped in ways that ensure activities are appropriate for their abilities? During a visit, observe whether residents are actively participating in programs or if they seem isolated or disengaged. Some facilities go a step further by offering sensory-focused options like Snoezelen rooms and tactile stations. These specialized spaces use interactive elements to create a more personalized and engaging experience, extending even to individual living spaces.
Personalization of Living Spaces
A familiar, homelike environment can make a significant difference in easing transitions and promoting well-being. Look for facilities that allow residents to customize their rooms with personal items like furniture, photos, linens, or even small pets (if permitted). Features like memory boxes outside rooms, color-coded hallways, or personalized door labels can also help residents navigate the space more independently.
Be mindful of the overall atmosphere during your visit. If living areas or common spaces feel sterile or overly clinical, it could be a red flag. Personal touches not only provide comfort but also help reduce confusion, making daily routines and transitions smoother for residents.
Common Areas and Recreational Spaces
Communal spaces are key to fostering social connections and mental stimulation. These areas should feel inviting and purposeful, avoiding an institutional vibe. Thoughtful design often includes clear sightlines to important amenities, which can help minimize confusion. Safety features, such as discreetly camouflaged exits and silent locks, should be seamlessly integrated into the environment.
Pay attention to details like noise levels (ideally between 55–70 dB), adequate lighting, and simple, calming décor, as these factors can significantly impact residents' comfort. Access to outdoor spaces is equally important. Secure courtyards and walking paths offer opportunities for sensory experiences and social interaction. Check that outdoor areas are easily accessible, free of barriers, and provide weather protection through natural shade or structures.
Some facilities also use a "human scale design" approach, grouping residents into smaller clusters of 6–15 individuals. This setup fosters a more intimate and socially engaging environment, making communal living feel less overwhelming and more personal.
Red Flags and Warning Signs
When evaluating care facilities, it's not enough to focus on safety measures alone. Even a place that looks perfect on the surface can hide serious issues. Knowing what to watch for during your visits can help you spot signs of neglect or poor care. Trust your gut - if something feels off, there's likely a reason.
Signs of Neglect or Poor Care
Start by observing the residents and their surroundings. Look for physical signs of neglect like unwashed hair, unpleasant odors, soiled clothing, unexplained injuries, bedsores, or sudden weight loss. These can indicate poor care or even abuse. Studies reveal that neglect and abuse are alarmingly common in such settings.
The facility's environment also tells a story. Persistent odors - whether from urine, feces, or overpowering cleaning agents - should raise alarms. As Margo Marasa, a Registered Nurse and Patient Advocate, points out:
"If an odor is present in the lobby, that can be cause for concern".
Look for signs of poor upkeep, such as dirt, clutter, or dim lighting, as these may also signal neglect. Pay attention to how staff interact with residents. If they seem rushed, annoyed, or unfamiliar with residents' names, it’s a red flag. Unanswered call lights or constantly ringing phones may suggest staffing issues.
Behavioral changes in residents are another clue. If they appear withdrawn, fearful, or agitated - especially around certain staff members - it’s worth investigating further. A lack of engaging activities, with residents left to sit passively in front of a TV, is also concerning. Jung Baccam, a Family Nurse Practitioner, advises:
"It's easy to get caught up in the shiny brochures and well-decorated rooms, but I encourage you to look beyond the surface".
Unannounced visits at various times of the day can provide a clearer picture of how the facility operates when they’re not expecting visitors.
Staff Reluctance to Answer Questions
Good facilities welcome questions and view families as partners in care. If staff seem defensive, hesitant, or rude when you ask questions, consider it a warning sign. Dr. Gary Small, Chair of Psychiatry at Hackensack University Medical Center, emphasizes:
"If you find they are unwilling to answer questions or they behave rudely, consider going elsewhere".
Be cautious if staff give vague answers about costs, tiered pricing, or extra fees for services like laundry or personal hygiene items. A reputable facility should provide clear documentation, such as their license, Resident Bill of Rights, and sample admission agreements. For Medicare- or Medicaid-certified facilities, they are legally required to share their most recent health inspection report upon request. Ask about staffing ratios during different shifts and emergency protocols - evasive answers could indicate deeper problems.
Environmental Concerns
Take a close look at the facility's physical condition and safety features. Broken equipment, malfunctioning smoke or carbon monoxide detectors, loose stair railings, slippery floors, or sudden changes in flooring can all pose risks. For residents with reduced sensory perception, water heaters should be set to 120°F or lower to prevent burns.
Pay attention to how quickly staff respond to call lights, as this reflects how well the facility is staffed. Inspect kitchen areas for expired food and confirm that stoves have safety features like automatic shut-offs. Also, ensure hazardous items such as medications and cleaning supplies are stored securely.
Conclusion
Choosing a dementia care facility is a deeply important decision. While many memory care facilities use advanced safety systems, those features alone don't guarantee quality care. Taking the time to evaluate thoroughly with this checklist can make all the difference in finding a safe, supportive environment versus one that might fall short.
Start your search early. As Eilon Caspi, Assistant Research Professor at the University of Connecticut, wisely points out:
"You don't want to wait for the crisis and then have 24 hours to make a decision".
Visit facilities unannounced and at different times of the day, such as mornings, mealtimes, and evenings, to get a genuine sense of how they operate. Go beyond surface impressions - request state inspection reports, test the handrails yourself, and talk to families of current residents for candid feedback. Staying vigilant ensures you’re prepared to adapt care as your loved one’s needs change.
Dementia is a progressive condition, so your involvement doesn’t stop after selecting a facility. Regularly review care plans to ensure they align with the evolving needs of your loved one. Keep up with visits, attend care meetings, and watch for red flags like frequent staff turnover or a decline in overall conditions.
Jill Lorentz, a Certified Dementia Trainer, emphasizes the importance of compassionate care:
"Look for caregivers who see your loved one as a person, not their disease. You want someone to help them thrive, not just survive".
With 78% of memory care communities offering specialized dementia training, you have every right to expect staff who are skilled and empathetic. If something feels off, don’t hesitate to dig deeper.
FAQs
What should I ask to confirm the facility can prevent wandering?
To ensure the safety of residents who may be prone to wandering, it's important to ask about the facility's security measures. Specifically, check whether they have a wander alert system in place and if outdoor areas are secured or locked to prevent unsupervised exits. You might ask questions like: "Does the facility have a wander alert system?" or "Are outdoor areas secured or designed to delay exits?" These precautions are essential for protecting residents with dementia.
How can I verify emergency response times and evacuation plans?
When choosing a facility, it's crucial to understand how prepared they are for emergencies. Start by asking about their emergency preparedness plan. Do they have a documented evacuation plan? If so, find out how often it’s updated and whether the staff receives regular training to stay ready for unexpected situations.
It’s also worth checking if they coordinate with local emergency services, like fire departments and paramedics. Ask if they conduct regular drills to ensure everyone knows what to do in a crisis.
Don’t stop there - review their licensing and inspection records to confirm they meet safety standards. If you can, visit the facility at different times to get a sense of how quickly staff responds to situations and how well evacuation procedures are communicated and practiced. Observing these details firsthand can give you valuable insights into their level of preparedness.
What red flags mean I should rule out a facility immediately?
Red flags to watch out for include residents who seem neglected - like being unkempt or wearing inappropriate clothing - and staff who appear rude, overwhelmed, or inattentive. Pay attention to the atmosphere: low participation in activities, noticeable clutter, unpleasant odors, and poor lighting can all indicate deeper problems. Additionally, frequent COVID-19 outbreaks or staff failing to respond quickly to residents' needs could signal issues with safety, cleanliness, or staffing levels. These warning signs may point to neglect or a lack of proper care.





